Resolving the Coronary Artery Disease Epidemic through Plant-Based
Nutrition - Present Heart Disease Management Strategies
Resolving the Coronary Artery Disease Epidemic through Plant-Based
Nutrition - Present Heart Disease Management Strategies
A Vegan Health Article from All-Creatures.org
These vegan health articles are presented to assist you in taking a pro-active part in your own health.
See All-Creatures.org Health Position and Disclaimer
From Caldwell B. Esselstyn, Jr., MD http://www.vegsource.com/esselstyn/
The present strategy focuses on interventional procedures and risk-factor modification. This approach is strictly a defensive strategy. It is pressing the limit of what society can afford. Our present cardiology budget exceeds one-quarter of a trillion dollars per year.1 Millions of symptomatic patients - generally those with arterial stenosis of more than 70% - have had interventions such as bypass, angioplasty, stenting, or atherectomy.13 Unfortunately, these interventions are accompanied by significant morbidity, mortality, and expense, provide only temporary benefit, and do nothing for patients at greatest risk for myocardial infarction, those with juvenile plaques of 30% to 50% stenosis, which are the ones most prone to rupture.14 As Forrester states, "angiography does not identify and interventional strategies don't treat those lesions most likely to cause a heart attack."15

Figure 1 -- Coronary angiograms of the distal left anterior descending artery before (left) and after (right) 32 months of a plant-based diet without cholesterol-lowering medication, showing profound improvement.
Therapies involving diet and lipid-lowering medication are not ignored by our health-care leaders, but sadly, their recommendations are clearly inadequate. The American Heart Association and the National Cholesterol Education Program (NCEP) recommend consumption of not more than 30% dietary fat and cholesterol levels below 200 mg/dL; numerous studies confirm that people who adhere to these recommendations experience not arrest and reversal of their heart disease, but rather continued disease progression.16 A question arises whether these recommendations expose millions to disease development and progression. However, because of the general respect commanded by these organizations, many doctors and patients perhaps are misled, trusting that following their recommendations will protect against heart disease.

Figure 2 -- Coronary angiograms of the circumflex artery before (left) and showing 20% improvement (right) following approximately 60 months of a plant-based diet with cholesterol-lowering medication.
The newer NCEP clinical guidelines, known as the Adult Treatment Panel 111, suggest broadening the identification of those at risk. This will mandate that millions of Americans take cholesterol-reducing drugs as well as make some dietary and physical activity adjustments. This is a rear-guard, after-the fact approach. It tacitly acknowledges that our food environment is so toxic that millions will become at risk and develop disease. As will be discussed, it is preferable to advise the public too avoid the categories of food that cause atherosclerotic disease.37
The National Research Council, in its 1989 report "Diet and Health," 17 recommended an upper limit of total cholesterol of 200 mg/dL and 30% dietary fat, even though "a number of the scientists felt that a greater reduction would confer additional health benefits."17 However, the committee felt that setting the cut-off too low would merely frustrate the public. The council also surmised, incorrectly, that if the upper level were set at 200 mg/dL, most Americans would achieve a total cholesterol level of 150 mg/dL or less.17 That has not happened. Most Americans and their physicians feel "safe" with a cholesterol total of up to 200 mg/dL. They are not. In the Framingham study, 35% of ischemic heart disease occurred in patients with total cholesterol levels between 150 and 200 mg/dL.18 In the CARE study, the average total cholesterol level in patients with a history of heart attack was 209 mg/dL.19 In contrast, the American Cancer Society recommends no more than 20% dietary fat,20 while the World Health Organization prefers no more than 15%.21
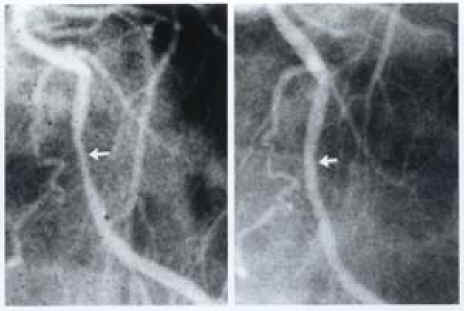
Figure 3-- Coronary angiograms of the proximal left anterior descending artery before (left) and showing 10% improvement (right) following approximately 60 months of a plant-based diet with cholesterol-lowering medication.
Dr. Scott Grundy, chairman of the NCEP, proclaimed approximately 14 years ago22 that 90% of heart attacks could be prevented if the population's cholesterol was 150 mg/dL or less - a figure identical to that hoped for by the National Research Council in 1989. However, neither the NRC, the American Heart Association, or the NCEP is on record to show precisely what diet will achieve the goal of cholesterol of 150 mg/dL. The basic diet favored by these groups contains not only grains, legumes, vegetables, and fruit, but also oil, low-fat milk and milk products, butter, cheese, poultry, lean meat, and fish. I am unaware of any research proving that by eating such a diet one can achieve a cholesterol level of 150 mg/dL or avoid coronary artery disease.
The Mediterranean diet and monounsaturated oils have become unjustifiably popular because of the Lyon Diet Heart Study.23 This approach is difficult to accept. No studies of monounsaturated oils have shown them to arrest and reverse coronary disease. The Lyon study did show a slower rate of progression, but this is hardly an acceptable goal. In a study of patients with coronary disease, Blankenhorn actually showed the reverse, that disease progressed as rapidly in patients on a monounsaturated diet as it did in those on a saturated fat diet.24 Rudel demonstrated a similar result in African green monkeys over a 5-year period.25 Particularly compelling was his finding that disease in the two groups was equivalent, even though the monounsaturated group had higher HDL, lower LDL, and more favorable LDL-to-HDL ratio. He recently replicated the results in rodents.26
The number of heart attacks continues to increase every year.27 Although the age-adjusted death rate for heart disease has declined, the decline may be artifactual.12 Stamler found deaths from cardiovascular disease approached 40% of those dying in a group of 80,000 young men with follow-up ranging from 16-34 years. The data confirmed a continuous graded relationship of serum cholesterol level to long term risk of coronary heart disease, cardiovascular disease, and all cause mortality. They also demonstrated substantial absolute risk and increased excess risk of coronary heart disease and cardiovascular disease death for younger men with elevated cholesterol levels and conversely a longer estimated life expectancy for younger men with favorable lipids.35 Our stop-gap, device-driven, risk factor-oriented approach is not working. Why? Because it fails to address our toxic food environment, which is responsible for the disease. It is focused only on those who are already ill or whose elevated lipids reflect an inability to detoxify their American diet. What are the other alternatives?
Go on to
Taking the Offensive
Return to
Resolving the Coronary Artery Disease Epidemic through Plant-Based Nutrition
Return to Vegan Health Articles
Visit Food Hazards in Animal Flesh and By-products
All-Creatures.org Health Position and Disclaimer
We began this archive as a means of assisting our visitors in answering many of their health and diet questions, and in encouraging them to take a pro-active part in their own health. We believe the articles and information contained herein are true, but are not presenting them as advice. We, personally, have found that a whole food vegan diet has helped our own health, and simply wish to share with others the things we have found. Each of us must make our own decisions, for it's our own body. If you have a health problem, see your own physician.